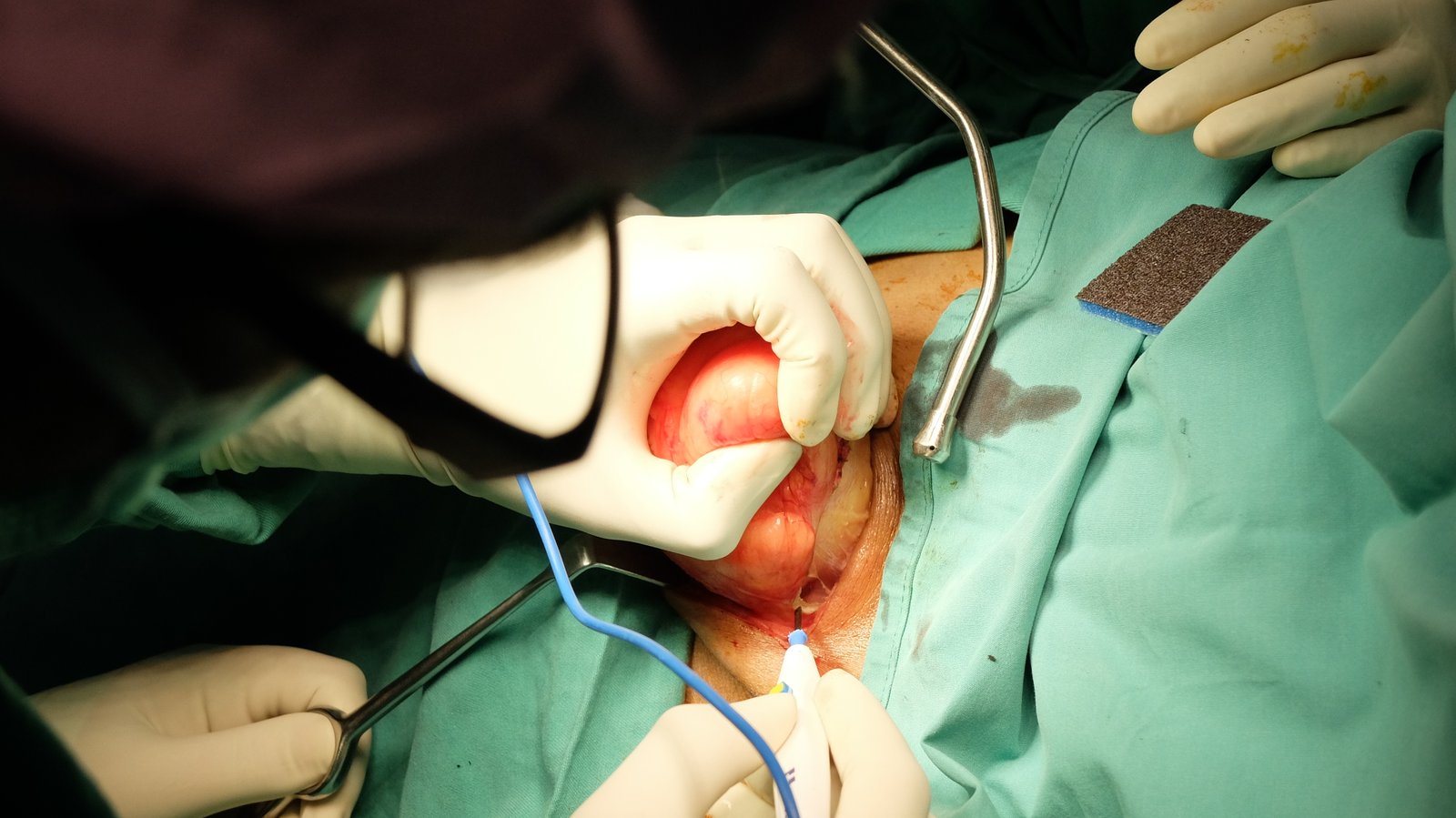
Open thyroidectomy surgery is a traditional procedure in which part or all of the thyroid gland is removed through an incision in the neck. It is commonly performed to treat thyroid cancer, large nodules, or other thyroid conditions. The surgery allows the surgeon direct access to the thyroid gland, ensuring precise removal of abnormal tissue while protecting surrounding structures such as nerves and parathyroid glands. It is a well-established and effective treatment option, especially in cases where advanced or complex thyroid conditions are present.
Open thyroidectomy is recommended in cases of thyroid cancer, large goiters, or nodules causing symptoms such as difficulty in breathing or swallowing. It is also preferred when minimally invasive options are not suitable.
Yes, open thyroidectomy is a safe and well-established surgical procedure when performed by an experienced surgeon. It has a high success rate and is widely used for effective treatment of thyroid conditions.
The procedure involves making a small incision in the front of the neck to access and remove the thyroid gland. The surgeon carefully preserves nearby structures such as nerves and glands to ensure safe outcomes.
Recovery time varies, but most patients can return to normal activities within 1–2 weeks. Complete healing may take a few weeks depending on the extent of surgery and individual health condition.
Yes, a small scar may be visible on the neck after surgery. However, surgeons usually place the incision in a natural skin crease to reduce its visibility over time.
Like any surgery, there are some risks such as infection, bleeding, or temporary voice changes. These risks are generally low and can be effectively managed with proper care. In rare cases, there may be temporary or permanent changes in calcium levels due to involvement of the parathyroid glands, or voice changes due to nerve irritation. However, with experienced surgeons and proper post-operative care, complications are uncommon and most patients recover safely without major issues.
Yes, if the entire thyroid gland is removed, patients may need lifelong thyroid hormone replacement medication. The doctor will guide you based on your condition and test results. These medications help maintain normal hormone levels in the body, ensuring proper metabolism, energy levels, and overall health. Regular follow-up and blood tests are important to adjust the dosage and ensure effective long-term management after surgery.